Abstract
Diabetes mellitus represents a heterogeneous group of metabolic disorders characterized by chronic hyperglycemia resulting from defects in insulin secretion, insulin action, or both. Its global prevalence continues to rise, posing substantial clinical and economic burdens. Contemporary management has evolved from a glucose-centric paradigm to a multifactorial, patient-centered approach incorporating cardiovascular risk reduction, weight management, and technological integration. This article provides a comprehensive overview of diabetes management, including pathophysiological mechanisms, diagnostic criteria, pharmacologic and non-pharmacologic interventions, and emerging therapeutic strategies.
Introduction
Diabetes mellitus affects over 500 million individuals worldwide and remains a leading cause of morbidity and mortality due to microvascular and macrovascular complications. The classification into type 1 diabetes (T1DM), type 2 diabetes (T2DM), and gestational diabetes reflects distinct but overlapping pathophysiological mechanisms. Modern management emphasizes individualized, outcome-driven care rather than uniform glycemic targets.
Pathophysiology of Diabetes Mellitus
T2DM arises from a complex interplay of insulin resistance and progressive β-cell dysfunction. Key mechanisms include impaired peripheral glucose uptake, increased hepatic gluconeogenesis, incretin dysfunction, and chronic inflammation.

4
Figure 1. Pathophysiology of Type 2 Diabetes Mellitus
Illustrates insulin resistance in muscle and adipose tissue, increased hepatic glucose output, and progressive β-cell failure.
In contrast, T1DM results from autoimmune-mediated β-cell destruction leading to absolute insulin deficiency.
Diagnostic Criteria and Glycemic Targets
Diagnosis is established through standardized biochemical thresholds:
- Fasting plasma glucose ≥126 mg/dL
- HbA1c ≥6.5%
- 2-hour OGTT glucose ≥200 mg/dL
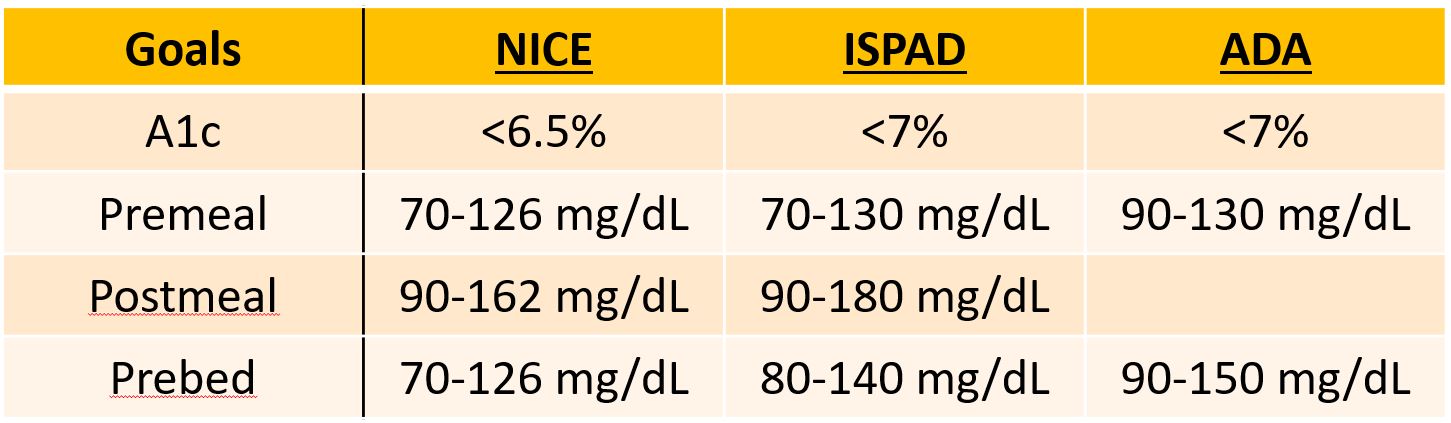
Glycemic targets should be individualized:
- HbA1c <7% (general population)
- Less stringent targets in elderly or comorbid patients


Non-Pharmacological Management
Lifestyle modification remains foundational:
- Structured dietary interventions emphasizing low glycemic index foods
- Regular physical activity (≥150 minutes/week)
- Weight reduction (5–10% improves insulin sensitivity)
Medical nutrition therapy (MNT) plays a critical role in long-term glycemic control.
Pharmacological Management
Treatment is individualized based on comorbidities and patient characteristics.
Major Drug Classes
- Metformin: First-line, reduces hepatic glucose output
- SGLT2 inhibitors: Provide cardiovascular and renal protection
- GLP-1 receptor agonists: Promote weight loss and improve glycemic control
- Insulin: Required in T1DM and advanced T2DM


4
Figure 3. Pharmacologic Treatment Algorithm
Stepwise intensification from monotherapy to combination therapy and insulin.
Insulin Therapy
Insulin remains the most potent glucose-lowering therapy and is essential in:
- T1DM
- Advanced T2DM
- Acute metabolic decompensation
Regimens include basal, bolus, and premixed insulin strategies.
Technological Advances in Diabetes Care
Continuous glucose monitoring (CGM) and insulin pump technologies have revolutionized diabetes care.
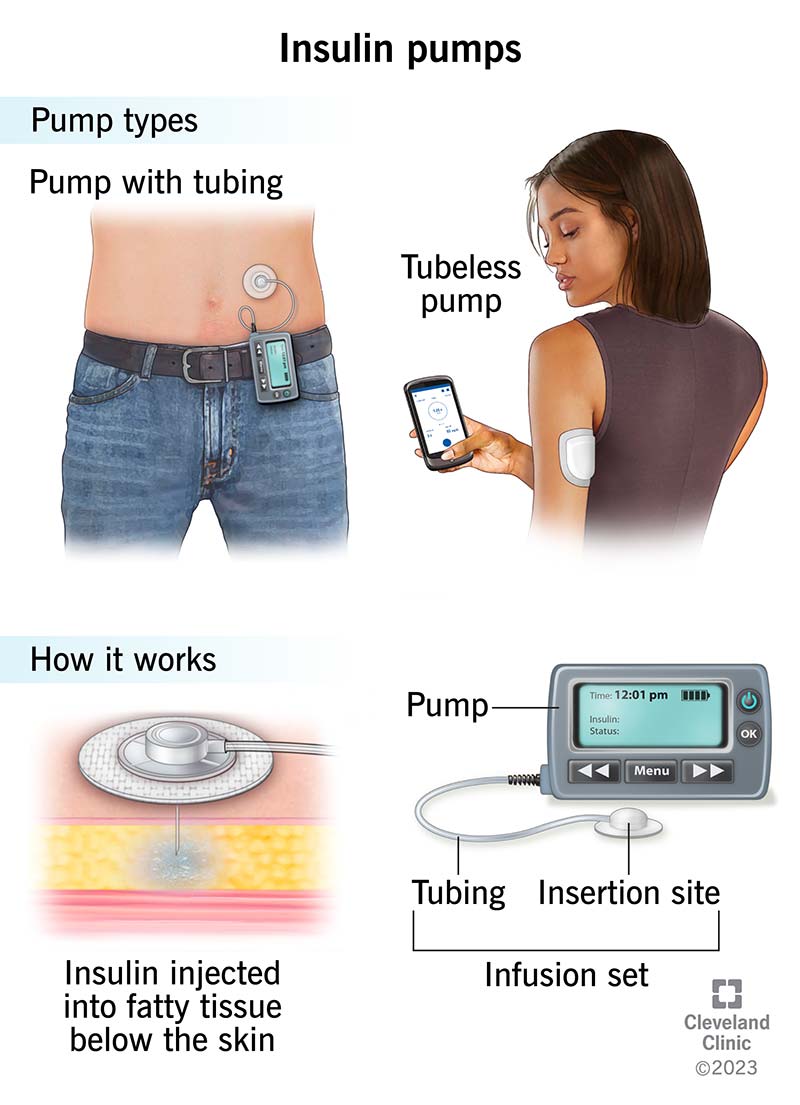
Shows real-time glucose trends and variability.
Management of Complications
Microvascular Complications
- Retinopathy
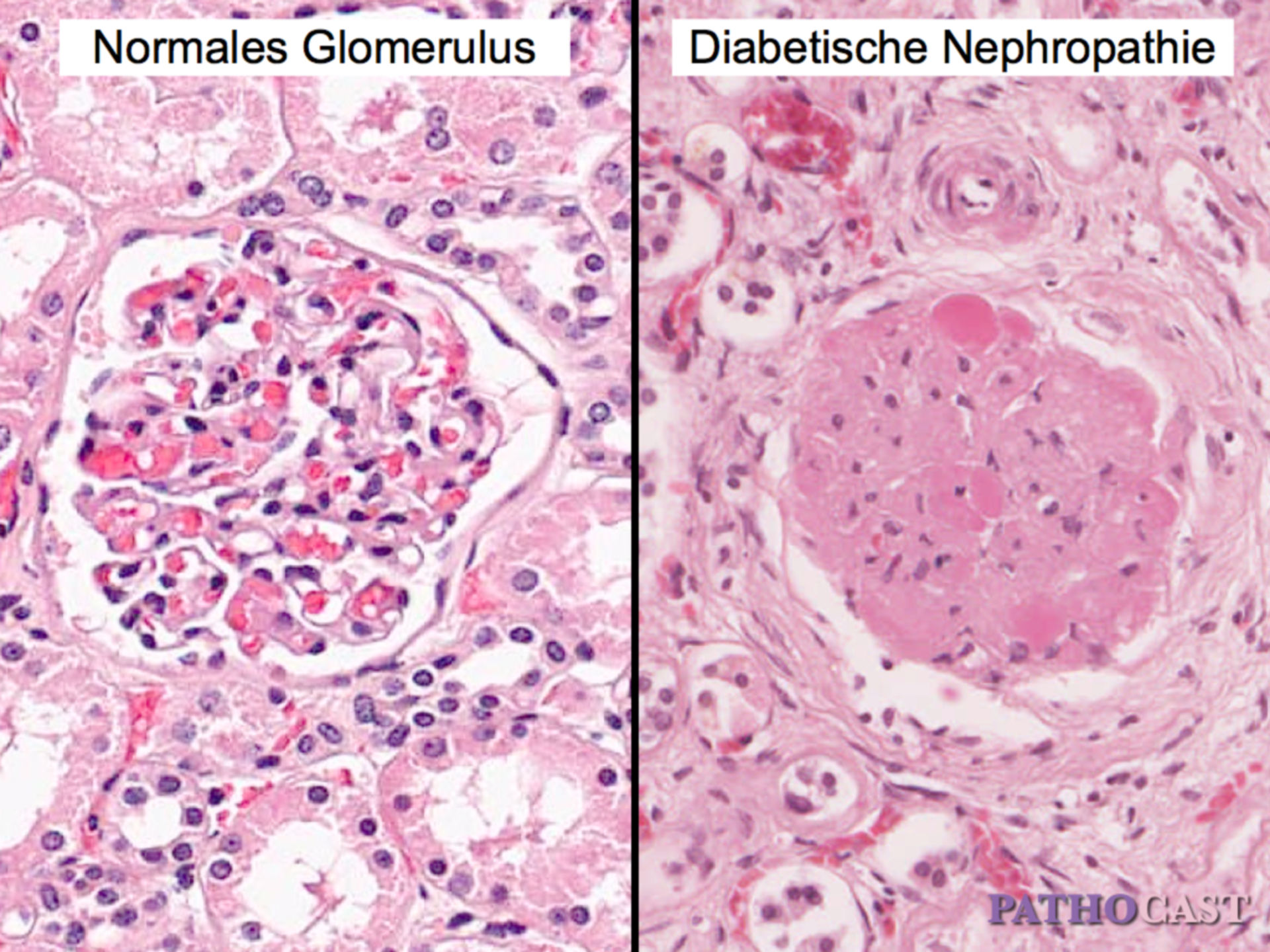
- Nephropathy
- Neuropathy


4
Microvascular Complications of Diabetes
Representative clinical manifestations including retinopathy and diabetic foot ulcers.
Macrovascular Complications
Cardiovascular disease remains the leading cause of mortality. Management includes aggressive control of:
- Blood pressure
- Lipids
- Lifestyle risk factors
Emerging Therapies and Future Directions
Recent advances include:
- Dual incretin receptor agonists (GLP-1/GIP)
- Stem cell–based β-cell replacement
- Precision medicine using genetic profiling
- AI-driven glucose prediction models
Discussion
Diabetes management has transitioned toward a comprehensive cardiometabolic model. Landmark trials such as UKPDS, EMPA-REG OUTCOME, and LEADER have demonstrated that certain antihyperglycemic agents confer benefits beyond glycemic control, particularly in reducing cardiovascular and renal outcomes.
Persistent challenges include therapeutic inertia, adherence barriers, and disparities in healthcare access.
Clinical Implications
- Personalized treatment strategies improve outcomes
- Early combination therapy may delay disease progression
- Technology enhances patient engagement and monitoring
- Cardiovascular risk reduction is central to management
Conclusion
Diabetes mellitus is a complex, chronic disease requiring a multifaceted and individualized approach. Advances in pharmacotherapy and technology have significantly improved outcomes, yet global disease burden continues to rise. Future directions emphasize precision medicine, disease modification, and equitable healthcare delivery.
References
- American Diabetes Association. Standards of Medical Care in Diabetes—2024. Diabetes Care.
- UK Prospective Diabetes Study (UKPDS) Group. Lancet. 1998.
- Zinman B, et al. EMPA-REG OUTCOME trial. N Engl J Med. 2015.
- Marso SP, et al. LEADER trial. N Engl J Med. 2016.
- Davies MJ, et al. Diabetologia. 2018.
- World Health Organization. Global Report on Diabetes.
- Buse JB, et al. Diabetes Care.


Leave a Reply